Journal of Emergency Medicine & Critical Care
Download PDF
Case Report
A “Drowning Miracle,” Case Study of a 2-Year-Old with Laryngospasms and Full Neurological Recovery. (Input from Video Surveillance and Clinician Bystander)
Kirupananthan A*
Sutter Health, San Francisco, CA, USA
Address for Correspondence:Anu Kirupananthan, Sutter Health, San Francisco, CA, USA. E-mail Id:
akirupananthan@gmail.com
Submission: 05 December 2024
Accepted: 03 March 2025
Published: 07 March 2025
Copyright: © 2025 Kirupananthan A. This is an open access article
distributed under the Creative Commons Attribution License, which permits
unrestricted use, distribution, and reproduction in any medium, provided the
original work is properly cited.
Abstract
Drowning, as defined by the World Health Organization, is the process of experiencing respiratory impairment due to submersion or immersion in liquid. Despite global efforts to prevent drowning, it remains the primary driver of deaths for children under 5 in the United States, and the third leading cause of accidental death worldwide, disproportionately affecting rural and low-to-middle-income areas [1-4].
Drowning outcomes range from mild respiratory impairment to severe neurological damage and death, known as fatal drowning. Immediate bystander intervention is essential in these cases, yet data on pre-hospital interventions are scarce. In 2-10% of drowning cases, laryngospasm occurs; a protective reflex in which the body forcibly closes the airways to prevent aspirate from entering the lungs [5]. While the primary injury from drowning is due to hypoxia, the extent to which laryngospasms contribute to this remains understudied, with limited literature on physiology or effective interventions [6,7].
One leading question from this case is whether there are clinical benefits of manual gastric decompression, also known as the Heimlich maneuver, during cardiopulmonary resuscitation (CPR) in a drowned victim with laryngospasms. This hypothesis was peripherally raised by Dr. Heimlich, who collected cases of drowning victims benefitting from the Heimlich maneuver. His theory that it cleared aspirate from the lungs was invalidated; however, this case proposes an alternative explanation. The Heimlich maneuver may benefit certain drowning victims by ejecting fluid and vomitus from the stomach, and decompressing the gastric space. In gastric distention, elevated abdominal pressure can impair ventilation and cardiac output by restricting lung expansion and decreasing venous return and cardiac output. Thus, safely decompressing the stomach may allow the vagus nerve to signal the superior laryngeal nerve to clear the laryngospasm and improve ventilation [5,7]. In emergencies where airway and perfusion are priorities, this approach could be lifesaving, especially when the risk of decompression aspiration is minimal by the completely closed airway in cases of laryngospasm [8].
In an emergency where optimal intervention focuses on airway and perfusion, could safely decompressing the stomach by inducing vomitus save lives? This case study aims to contribute to the ongoing discussion and research on this critical issue, which has profound social implications for families and communities.
Drowning outcomes range from mild respiratory impairment to severe neurological damage and death, known as fatal drowning. Immediate bystander intervention is essential in these cases, yet data on pre-hospital interventions are scarce. In 2-10% of drowning cases, laryngospasm occurs; a protective reflex in which the body forcibly closes the airways to prevent aspirate from entering the lungs [5]. While the primary injury from drowning is due to hypoxia, the extent to which laryngospasms contribute to this remains understudied, with limited literature on physiology or effective interventions [6,7].
One leading question from this case is whether there are clinical benefits of manual gastric decompression, also known as the Heimlich maneuver, during cardiopulmonary resuscitation (CPR) in a drowned victim with laryngospasms. This hypothesis was peripherally raised by Dr. Heimlich, who collected cases of drowning victims benefitting from the Heimlich maneuver. His theory that it cleared aspirate from the lungs was invalidated; however, this case proposes an alternative explanation. The Heimlich maneuver may benefit certain drowning victims by ejecting fluid and vomitus from the stomach, and decompressing the gastric space. In gastric distention, elevated abdominal pressure can impair ventilation and cardiac output by restricting lung expansion and decreasing venous return and cardiac output. Thus, safely decompressing the stomach may allow the vagus nerve to signal the superior laryngeal nerve to clear the laryngospasm and improve ventilation [5,7]. In emergencies where airway and perfusion are priorities, this approach could be lifesaving, especially when the risk of decompression aspiration is minimal by the completely closed airway in cases of laryngospasm [8].
In an emergency where optimal intervention focuses on airway and perfusion, could safely decompressing the stomach by inducing vomitus save lives? This case study aims to contribute to the ongoing discussion and research on this critical issue, which has profound social implications for families and communities.
Introduction
Case Study:
On a hot June Saturday afternoon, a 33-month-old, 10 kg female
was found submerged in the shallow end of a residential pool. The
pool, prepared for pediatric swim lessons, was freshly cleaned and
maintained at 30°C, with active water filtration and heating, creating
a gentle current.Security footage revealed the child was unconscious for eight
minutes before intervention. In the minutes leading up to this, she
is seen in a sleeved rash guard swimsuit with neck coverage, opening
the front door, a newly acquired skill, and firmly closing it behind
her. She proceeded to the garage, attempting but failing to open the
heavy child-proof door leading to the pool. Undeterred, she exited
the garage and accessed the pool area through a side entry gate of a 5.5
feet fence. A bell had been attached to the latch to notify opening and
closing, but this prevented the door latch from fully closing.
The child cautiously walked by the deep end of the pool, stepped
over a garden hose, and approached the shallow end. She placed one
foot on the first stair, five inches below the water’s surface, followed
by the other foot while holding the pool’s cement rim. She splashed
with one hand. Then, as she placed both hands into the water, she
floated up and pulled away from the steps. After 20 seconds, her face
submerged, and within a minute, she ceased movement.
She remained submerged for eight minutes before being pulled
out and CPR initiated. Another adult assisted and called 911,
notifying the emergency room team to prepare for her arrival at a
regional trauma center, five minutes away.
After two rounds of 30 compressions to 2 breaths, the 2-year-old
was moved to the floor of a van and transported to the Emergency
Department (ED) with continued CPR delivery. No foam was noted
at any point during CPR.
The clinician bystander performing CPR observed that airway
management was initially ineffective. Despite tilting the head back,
clasping the nostrils closed, and delivering breaths through a tight
seal over the mouth, there was no chest rise. The breaths felt “like
blowing on a brick wall.”
After two more rounds of ineffective large forceful breaths,
but strong compressions, the bystander delivered a prolonged
breath, accidentally inducing vomiting. The subsequent breath “felt
effective,” and had some minimal chest rise. After another round
of compressions, they repeated the prolonged large breath, turned
the child to the left, concurrently pushing up on the stomach, and
manually induced the expulsion of a large bolus of water and food
remnants.
The bystander repeated this process while adjusting CPR to a
15:2 compression-to-breath ratio for the remainder of the drive
(approximately 4 minutes). At this point, each breath resulted in
chest rise without resistance.
Upon arrival at the ED, the child was found to be in normal
sinus rhythm with agonal breathing. She was immediately intubated,
placed on a cervical collar and transferred to the local Children’s
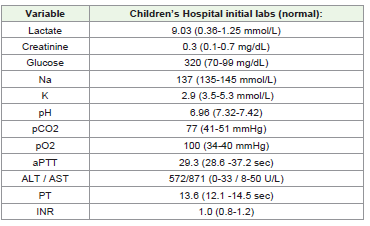
Hospital Pediatric Intensive Care Unit (PICU). The results of initial
hematologic laboratory tests are shown in [Table 1].
Within two hours of her initial labs, her lactate improved to 4.63
mmol/L, and within 5 hours dropped to a normal of 0.96 mmol/L.
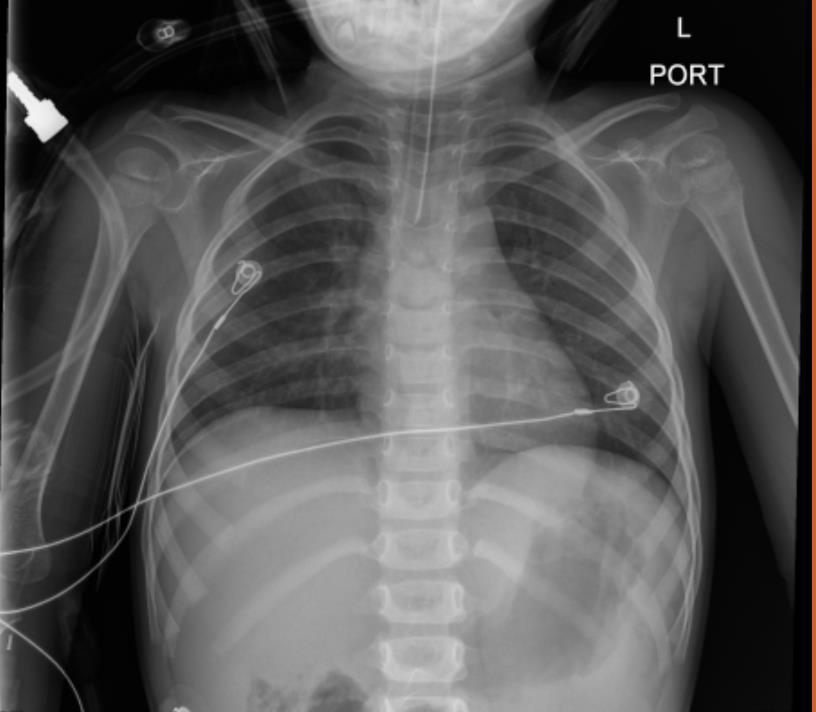
Initial chest X-ray was unremarkable with minimal atelectasis and
gaseous distention [Figure 1]. Her CT scan was benign.
She was enrolled in the Pediatric ICECAP study and randomized
to 72 hours of induced hypothermia at 33°C [9]. She was placed on
delirium prevention and infection prevention measures, including
maintaining her sleep and nap schedules. Team members entering
her room were asked to wear masks as the induced hypothermia
dropped her WBC to 1.6 thousand/mm3 (normal 5-14 thousand/
mm3).
Her PICU course was uncomplicated. There were no seizures, delirium, infection or pneumonitis.
After 72 hours, she was rewarmed and underwent a normal magnetic resonance imaging (MRI). She was successfully extubated on the first attempt, remarked ‘I’m so silly,’ and proceeded to eat three ice pops.
Her PICU course was uncomplicated. There were no seizures, delirium, infection or pneumonitis.
After 72 hours, she was rewarmed and underwent a normal magnetic resonance imaging (MRI). She was successfully extubated on the first attempt, remarked ‘I’m so silly,’ and proceeded to eat three ice pops.
She then awaited transfer to inpatient pediatric rehabilitation.
Within 48 hours, she was walking with assistance, communicating
in two languages, eating solid foods, and maintaining her sleep
schedule. The child was discharged home with continued monitoring
from physical, speech, and occupational therapy. At 12 weeks, she
was classified as Level 1 on the Pediatric Overall Performance
Category Scale, indicating ‘Good overall performance: healthy, alert,
and capable of normal activities of daily life[10].
Discussion
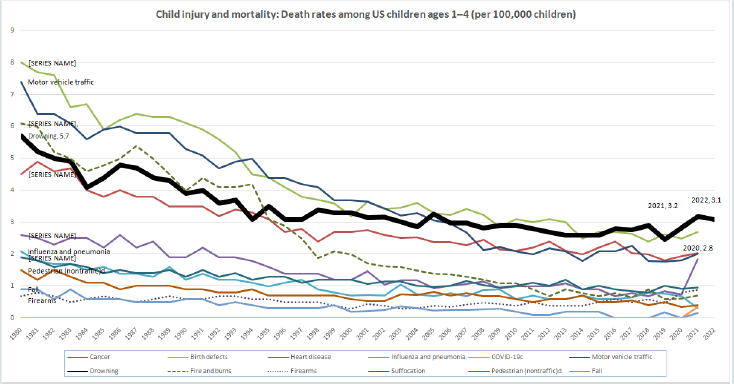
Drownings are currently the leading cause of mortality in young
children in the United States [1-4] [Figure 2]. Since 1995, drowning
has surpassed fires and burns as the primary source of death for
children aged 4 and under, largely because rates of deaths from
fires have declined. However, since 2020, there has been a marked
increase in pediatric drowning cases. For every fatal drowning, it is
estimated that 4 non-fatal victims seek care [11]. Adult supervision,
early swimming lessons, pool fencing, and pool covers are effective
measures to prevent drowning incidents [3]. When drowning
cannot be prevented, factors such as submersion time, bystander
intervention, the need for and initiation of advanced life support,
the duration of CPR, and the return of spontaneous breathing are
crucially correlated with survival and neurological outcomes [12].
The drowning victim may have multi-factorial elements for
causing physiological dysfunction including cardiopulmonary
response to both temperature and hypoxia. Despite the victim
attempting to hold their breath, coughing and involuntary
laryngospasms occur. Recent studies have shown that laryngospasms
resulting from drowning are always complete[8]. With the closure of
the vocal cords, water enters the gastrointestinal tract. This protective
mechanism is thought to last for approximately one minute. However,
in 20% of cases, laryngospasms continue even after cardiac arrest.
Laryngospasms are also 2-3x more common in younger children [13].
When the laryngospasms cease, water then enters the respiratory
tract causing bronchospasms. This often causes foam from cellular
damage to alveolar walls and surfactant washout. This foam may be
beneficial and can be bagged back into the lungs. Cardiac dysfunction
can occur at any of these points, and it follows a predictable hypoxic
pattern: sinus tachycardia, bradycardia, pulseless electrical activity
then asystole. While any organ can see injury, the most susceptible
areas to ischemic injury are vascular end zones. In the brain, these
are often the hippocampus, insular cortex, and basal ganglia. More
severe hypoxic-ischemic events result in more extensive and global
neocortical injury [14,15].
Drowning may cause a significant amount of water to enter the
stomach (approximately 500 mL in a 2-year-old and up to 4 liters
in adults). In many cases where CPR is administered, CPR can also
induce vomiting. However, the drowned victim that does not respond
needs airway, breathing and circulation (ABC) management as
quickly as possible, as opposed to the typically practiced circulation airway-
breathing (CAB) pathway per the 2024 American Heart
Association, American Academy of Pediatrics Focused Update and
International Guidelines [15-21]. If CPR induces vomiting, sweeping
the vomitus away, and continuing CPR is prioritized.
Conclusion
The pathophysiology of drowning is complex, and there is a
significant need for more research in this field. We do not fully
understand how the body responds to submersion and immersion,
including why some victims have laryngospasms, and other do not.
We also neither have physiological data on laryngospasms, nor do
we have clear epidemiological data on outcomes of resuscitation in
this population. This lends to a gap in our understanding of the most
appropriate resuscitation mechanism for these victims [7,16,22].
The field of Anesthesia has published the most on laryngospasms
in the field of post-surgical risks and complications, and gives us our
biggest window of exploring other options. In post-op cases, young
children have thrice the risk of laryngospasms as older children.
Laryngospams are managed by medications, through jaw thrusts
or using Larson’s maneuver [13]. Jaw thrusts pull the vocal cords
apart, and may be easily taught to bystanders. Larson’s maneuver,
while effective, may be more difficult to perform in the field by
untrained persons. In using medications to manage laryngospasms,
there is a preference to quickly deepen anesthesia using Propofol and
Succinylcholine, and perform gastric decompression to maintain the
open airway [23].
81% of fatal drownings involving US children under age 15
occurred in a residential setting, including at the victim’s home,
the home of a family member, friend, or neighbor[20]. Even in the
United States, where Emergency Medical Services are available, it
can take an average of 7-14 minutes for EMS to arrive on scene at
a life-threatening emergency. And if EMS then decides to intubate,
field intubation only has a 60% success rate, with no data available
on successful intubation rates for laryngospasms[21,24,26]. In many
of these cases, intubation at the scene will be difficult, or futile (in the
case of laryngospasms). Any resources we can provide to bystanders
and first responders in these dire situations can have meaningful
impact.
Dr. Henry Heimlich collected intervention stories when the
Heimlich maneuver was used, and inadvertently found cases where
drowning victims potentially benefitted. He hypothesized that subdiaphragmatic
thrusts, or the Heimlich maneuver, could help clear
liquid from the esophagus and lungs in drowning victims. Though a
1993 review by the Institute of Medicine found no evidence that the
maneuver could clear aspirate from the lungs to improve ventilation
and oxygenation, it is possible that Dr. Heimlich’s observations may
still hold value [5].
This case proposes an alternative explanation: the Heimlich
maneuver, or gastric decompression, may benefit certain drowning
victims by ejecting fluid and vomitus from the stomach and
decompressing the gastric space. In gastric distention, elevated
abdominal pressure can impair ventilation and cardiac output by
restricting lung expansion and decreasing venous return and cardiac
output. Thus, safely decompressing the stomach might allow the
laryngospasm to clear and improve ventilation. In emergencies where
airway and perfusion are priorities, this approach could be lifesaving,
especially when the risk of aspiration is minimal by the completely
closed airway in cases of laryngospasm [9].Perhaps, intentional
gastric decompression in the recovery position can even reduce the
likelihood of aspiration pneumonia in post-drowning laryngospasms.
This drowning miracle case, suggests that laryngospasm may
have been alleviated through forced gastric emptying, facilitating
diaphragmatic relaxation and airway opening. Perhaps this can be
an additional tool in CPR to increase the window of opportunity in
airway management, in one of the most devastating international
public health challenges we face.
Acknowledgements:
A gracious thank you to the family, bystander, clinical team and
2024 Western States Advocacy Committee Chair of the American
Heart Association.